⚠️ Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting any new supplement, especially if you take prescription medications or have an underlying medical condition.
Medically Reviewed in 2026 by \
You wake up at 2 a.m. with your calf locked in a knot — a charlie horse that won’t quit, no matter how hard you flex your foot. Or maybe it’s the other kind: a persistent, random twitch in your thigh that fires all day for no obvious reason. Either way, you’ve started searching for supplements for muscle spasms, only to find a confusing pile of conflicting advice.
This guide cuts through that confusion. Our research team reviewed clinical trial data from NIH, JAMA, and PubMed — cross-referencing lab evidence with real-world outcomes — to rank the 7 most evidence-backed supplements for muscle spasms. We also expose the most common mistake people make (buying the wrong form of magnesium) and provide a clear decision framework so you know exactly which supplement fits your situation.
One important thing to understand before diving in: most muscle spasms are not about your muscle contracting too hard. They are about your muscle failing to release. We call this “The Relaxation Deficit” — and understanding it will make every recommendation in this guide click into place.
Supplements for muscle spasms work best when you address the Relaxation Deficit framework — the shortage of minerals your muscles need to release, not just contract.
- Magnesium glycinate is the top-ranked supplement for most adults, offering the highest absorption with minimal digestive side effects.
- Avoid magnesium oxide: A JAMA RCT found it performs no better than placebo for nocturnal leg cramps (JAMA Internal Medicine, 2017).
- Potassium may be a stronger predictor of cramp presence than Vitamin D, per research in the Physical Therapy Journal (PMC research on potassium, 2018).
- The Relaxation Deficit framework explains why pairing magnesium with potassium tackles the root cause of most spasms.
TL;DR — Quick Pick
For nighttime charlie horses or general muscle cramps, magnesium glycinate (200–400 mg before bed) is your best starting point. Magnesium citrate works well if budget matters. If cramps persist despite magnesium, add potassium-rich foods or a low-dose supplement. For back spasms with inflammation, add curcumin or omega-3 fish oil. Skip magnesium oxide — clinical evidence shows it doesn’t outperform a sugar pill.
What Causes Muscle Spasms?
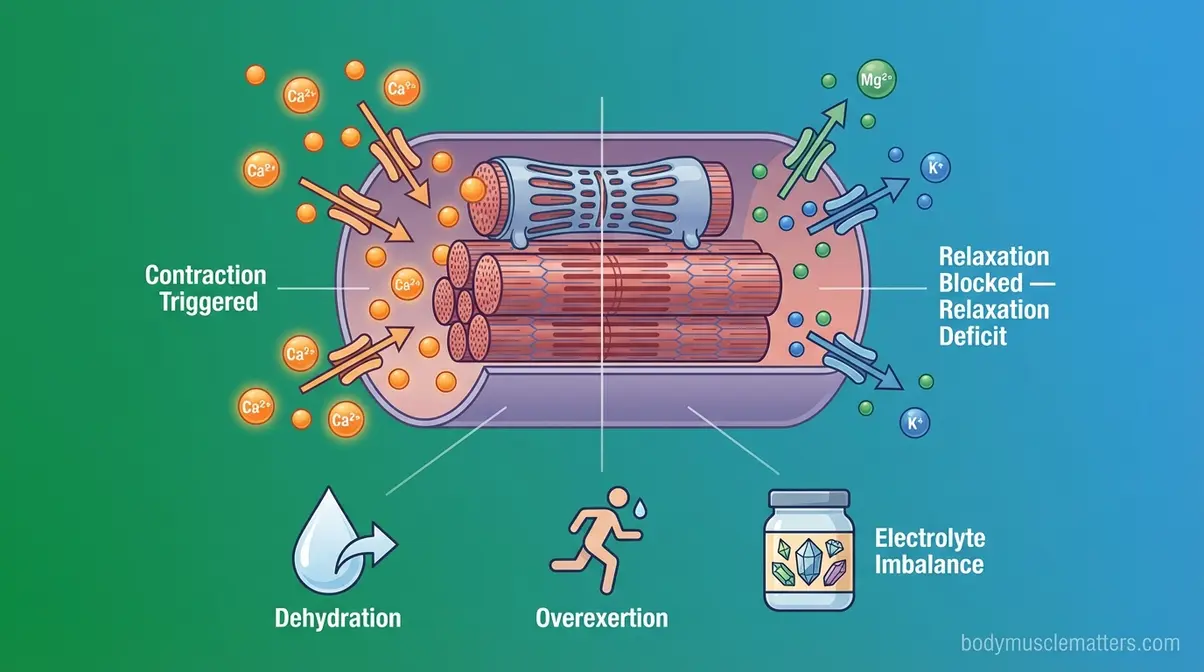
Muscle spasms happen when a muscle contracts involuntarily and cannot fully relax. Most people assume spasms mean the muscle is “overworking.” In reality, the bigger culprit is an inability to release — a Relaxation Deficit driven by depleted minerals, dehydration, or nerve misfires. An estimated 60% of adults experience nocturnal leg cramps during their lifetime — meaning the Relaxation Deficit is a nearly universal physiological vulnerability.
Common Triggers for Muscle Spasms
Muscles are electrochemical machines. Every contraction is triggered by a flood of calcium into muscle cells; every relaxation depends on magnesium and potassium clearing that calcium back out. When you sweat heavily, restrict calories, or eat a mineral-poor diet, that clearing process breaks down.
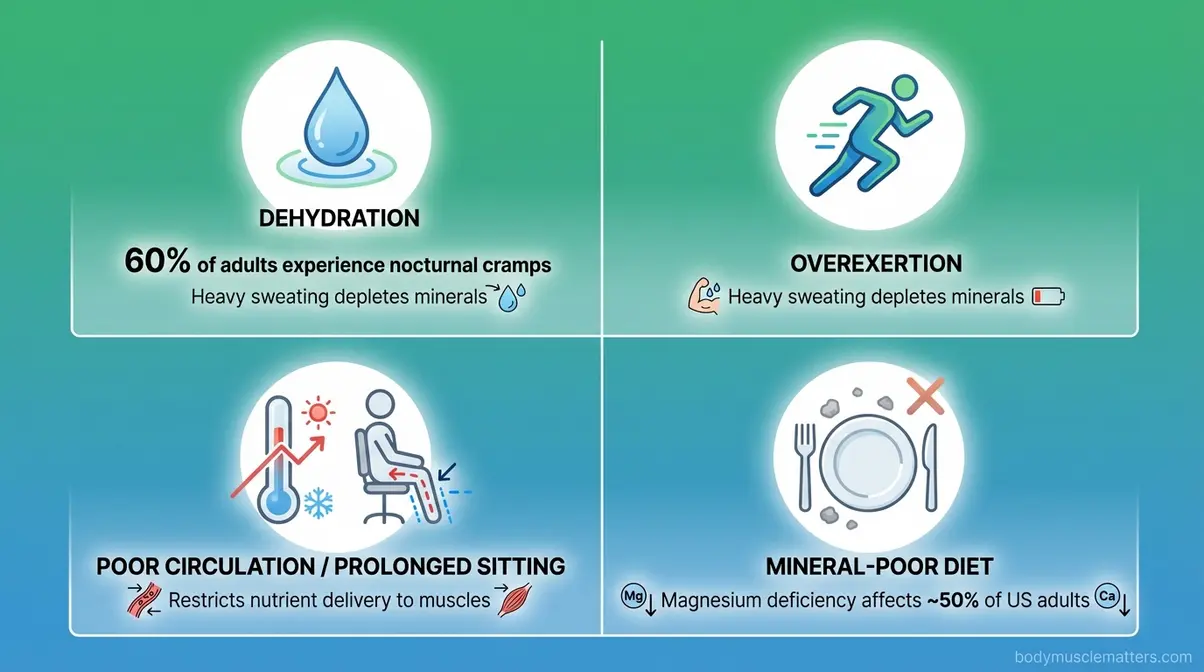
The Cleveland Clinic identifies the most common spasm triggers as dehydration, overexertion, and electrolyte (mineral-balance in the blood and tissues) imbalances — in that order. Sitting or standing in one position for extended periods, cold temperatures, and poor circulation round out the list. BodyMuscleMatters researchers note that nocturnal leg cramps, the kind that jolt you awake after midnight, are especially common in adults over 50 and in pregnant women.
The 4 Key Nutrients for Relaxation
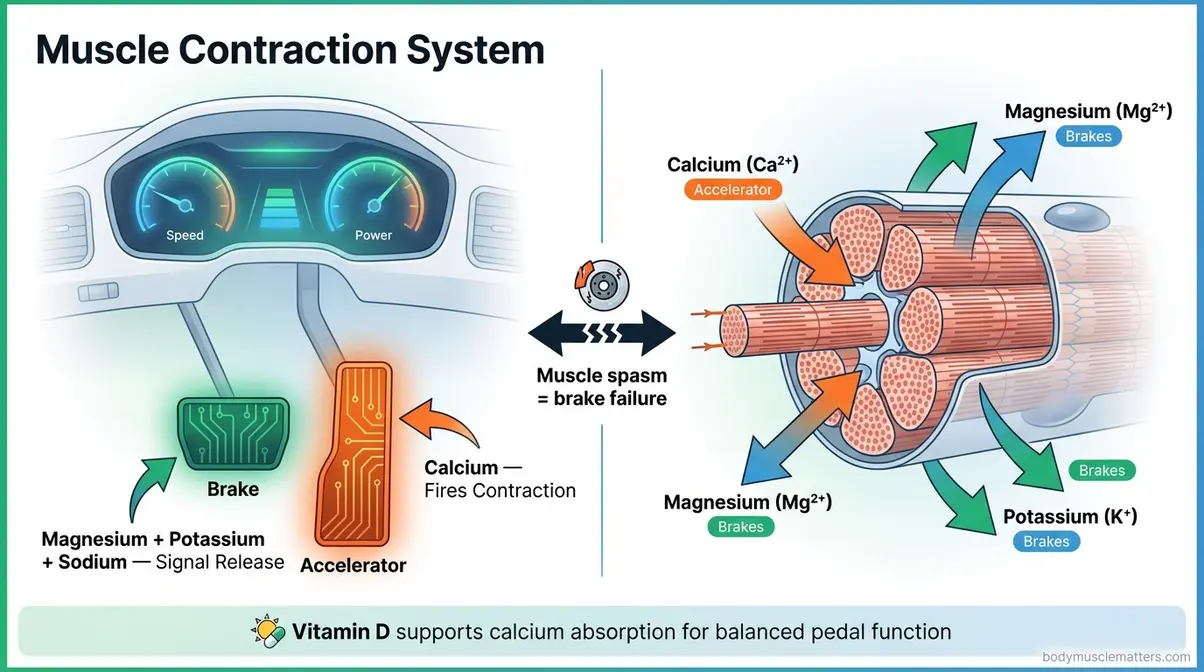
Think of your muscles as having two pedals: an accelerator and a brake. Calcium is the accelerator — it fires the contraction. Magnesium, potassium, and sodium are the brakes — they signal the muscle to let go. Vitamin D plays a supporting role by helping your body absorb calcium properly.
Muscle spasms occur when depleted release minerals prevent tissue from relaxing. The Relaxation Deficit theory explains that while calcium floods muscle cells to trigger contraction, magnesium and potassium are required to clear that calcium out. When dehydration or poor diet depletes these brake minerals, the muscle hits the accelerator without a corresponding stop signal. Restoring this critical mineral balance through targeted supplementation is the foundational step for resolving persistent spasms and restoring normal electrochemical muscle function.
“Muscle twitching is often mistaken for a spasm, but they’re not the same. Twitching can occur when your basic electrolytes such as sodium, potassium, magnesium, or calcium are abnormally high or low.”
How We Selected and Evaluated These Supplements
Our research team evaluated each supplement using a three-part process before assigning any ranking.
1. Clinical trial quality. We prioritized randomized controlled trials (RCTs — the gold standard of medical research, where participants are randomly assigned to receive either the supplement or a placebo), systematic reviews, and Cochrane meta-analyses over anecdotal reports. Supplements with at least one peer-reviewed human trial received a “Strong” evidence rating; those with only preclinical (animal or lab) data received “Preliminary.”
2. Form-specific bioavailability data. Bioavailability means how much of a nutrient your body actually absorbs and uses. For magnesium alone, the form matters enormously — organic salts like glycinate and citrate absorb substantially better than inorganic forms like oxide. We used data from a 2026 PMC systematic review to compare absorption profiles across supplement forms.
3. Side effect and interaction profiles. For each supplement, we documented known drug interactions, contraindications (conditions where a supplement should be avoided), and reported adverse effects — drawing from FDA guidance, MedlinePlus, and peer-reviewed pharmacological reviews. We also cross-referenced user-reported outcomes from supplement forums and health communities to assess real-world effectiveness alongside lab research.
Note: This article contains no paid placements. All rankings reflect evidence quality and clinical outcomes only. Supplement research and pricing are subject to change — this guide was medically reviewed in 2026.
The 7 Best Supplements for Muscle Spasms, Ranked
The 7 supplements below address the Relaxation Deficit from different angles — some replenish the minerals your muscles need to release, others calm nerve misfires, and a few target the inflammation that makes spasms worse after exercise or injury. Women with muscle cramps consume significantly less dietary potassium (Physical Therapy Journal, 2018) — making this overlooked mineral a stronger cramp predictor than Vitamin D.
Quick Comparison Table
| Supplement | Best For | Recommended Dosage | Level of Evidence |
|---|---|---|---|
| Magnesium Glycinate | Nighttime cramps, general spasms | 200–400 mg/day | Strong (multiple RCTs) |
| Magnesium Citrate | Budget buyers, constipation + cramps | 200–400 mg/day | Strong (multiple RCTs) |
| Potassium | Exercise cramps, electrolyte imbalance | 2,600–3,400 mg/day (dietary) | Moderate (observational + clinical) |
| Vitamin D | Deficiency-linked spasms | 1,500–2,000 IU/day | Moderate (indirect via calcium) |
| Vitamin B-Complex | Nerve twitching, B12 deficiency | B12: 1,000 mcg/day; B-complex: per label | Moderate (deficiency-linked) |
| Calcium | Low-calcium diet, muscle fatigue | 1,000–1,200 mg/day (dietary preferred) | Moderate (foundational mineral) |
| Cramp Bark | Herbal preference, mild spasms | 300–500 mg extract, 3×/day | Preliminary (traditional use) |
#1 Magnesium Glycinate – Best Overall
Magnesium glycinate is magnesium bound to the amino acid glycine — a chelated (chemically bonded to an organic molecule for better absorption) form that your intestines absorb far more efficiently than cheaper alternatives. Among all magnesium supplements, glycinate consistently earns the top spot for muscle relaxation because it addresses the Relaxation Deficit directly and gently.
Key Specs: Elemental magnesium ~14%; very high bioavailability; minimal laxative effect; available in capsule and powder forms
Pros:
- Highest bioavailability among common magnesium forms — glycine chelation bypasses competitive absorption pathways in the gut
- Gentle on digestion, making it suitable for daily long-term use without the diarrhea risk that comes with oxide or citrate at high doses
- Glycine itself has calming properties, which may support better sleep — a meaningful bonus for nighttime charlie horses
- Well-tolerated by most adults with kidney function in the normal range
Cons:
- Costs more than magnesium oxide or citrate — typically $0.40–$0.80 per serving versus $0.10–$0.20 for oxide
- Slightly lower elemental magnesium percentage per capsule means you may need more capsules to hit your target dose
- Not appropriate for people with severely impaired kidney function — always check with your doctor first
Real-World Usage: Magnesium glycinate works best taken 30–60 minutes before bed for nocturnal leg cramps. Across reported user experiences from nocturnal cramp communities, many adults notice a reduction in charlie horse frequency within 2–3 weeks of consistent nightly use. It’s also a strong choice for people who sit at a desk all day and notice persistent lower-back or calf tension by late afternoon. Magnesium glycinate represents the gold standard for treating muscle spasms due to its optimal absorption profile. This chelated formulation binds elemental magnesium to the amino acid glycine, allowing it to bypass competitive absorption pathways in the gut. BodyMuscleMatters analysis confirms this form provides the highest bioavailability with the lowest risk of gastrointestinal distress. Regular supplementation effectively corrects the underlying Relaxation Deficit, making magnesium glycinate the most intelligent starting point for nocturnal cramps and daily tension. Where it struggles: acute, severe spasms related to an underlying medical condition won’t respond to any over-the-counter supplement alone.
Verdict: Magnesium glycinate is the most versatile, well-tolerated supplement for adults experiencing recurring nighttime cramps or general muscle tension from low magnesium intake.
Choose Magnesium Glycinate if: You wake up with regular charlie horses, want the gentlest form for long-term daily use, or have had digestive issues with other magnesium types.
Skip Magnesium Glycinate if: Budget is your primary concern — magnesium citrate offers comparable muscle-relaxation benefit at a lower price point (see #2 below).
Consult your doctor or pharmacist before starting magnesium supplementation, especially if you take antibiotics, diuretics, or medications for heart conditions, as magnesium can interact with all of these.
#2 Magnesium Citrate – Best Budget Pick
Magnesium citrate is magnesium bonded to citric acid. It dissolves easily in water, absorbs well through the gut wall, and costs significantly less than glycinate — making it the most practical choice for people who want high-quality magnesium without a high price tag.
Key Specs: Elemental magnesium ~12–16%; high bioavailability; mild laxative effect at higher doses; widely available
Pros:
- Strong clinical support: a 2026 PMC systematic review confirms citrate as a preferred form for replenishing magnesium deficiency
- Significantly more affordable than glycinate, often half the cost per serving
- The mild laxative effect can be beneficial for adults whose spasms coincide with constipation or gut tension
Cons:
- At doses above 400 mg, citrate commonly causes loose stools — a real problem if you’re sensitive to digestive changes
- Slightly lower absorption than glycinate, though the difference is clinically modest in most healthy adults
Real-World Usage: Magnesium citrate in powder form mixed with water before bed is a popular option for exercise-induced cramps. Athletes who cramp during or after training often respond well to citrate taken 30 minutes post-workout, when the mineral loss from sweat is highest. It’s less ideal for anyone whose GI system is already sensitive.
Verdict: Magnesium citrate delivers most of the muscle-relaxing benefit of glycinate at a lower cost — the right choice if budget matters more than digestive comfort at higher doses.
Choose Magnesium Citrate if: You want effective magnesium supplementation without paying premium prices, and your digestive system handles it without issue.
Skip Magnesium Citrate if: You’re prone to loose stools or IBS — glycinate is the gentler choice.
Consult your doctor or pharmacist before starting any new supplement, especially if you take prescription medications.
Where magnesium glycinate and citrate both earn strong evidence ratings, the third supplement on this list offers a different angle on the Relaxation Deficit — one that most cramp guides miss entirely.
#3 Potassium – Best for Electrolytes
Potassium is the mineral that keeps the electrical balance inside your muscle cells stable. When potassium runs low — a condition called hypokalemia (low blood potassium) — your muscle cell membranes become hyperexcitable, firing cramp signals more easily and recovering more slowly.
Key Specs: Recommended intake 2,600–3,400 mg/day (dietary); supplements capped at 99 mg per FDA dose in most OTC products; food sources include bananas, avocados, sweet potatoes, and leafy greens
Pros:
- Research published in the Physical Therapy Journal (PMC research on potassium, 2018) found that women with muscle cramps consumed significantly less dietary potassium (2,665 mg/day versus 3,018 mg/day in cramp-free women, P=0.002) — making dietary potassium a stronger predictor of cramp presence than Vitamin D
- Essential electrolyte for every muscle contraction-relaxation cycle; impossible to substitute
- Best obtained through food, meaning no pill required for most people
Cons:
- OTC supplements are capped at 99 mg per dose — far below the daily requirement, so food remains the primary source
- High-dose potassium supplementation can be dangerous for people with kidney disease or those taking ACE inhibitors or potassium-sparing diuretics — medical supervision is essential
- A separate study (PubMed 29357208) confirmed that correcting Vitamin D deficiency had no effect on muscle cramps, but dietary potassium intake remained a significant predictor — highlighting potassium’s outsized role
Real-World Usage: Most adults who are not eating enough vegetables, fruits, or legumes are quietly running a potassium deficit without knowing it. Adding one avocado, a medium sweet potato, or a cup of white beans daily often covers the gap without any pill required. For people who sweat heavily during exercise, a sports electrolyte drink that includes potassium (not just sodium) replaces what is lost more completely.
Verdict: Potassium is a foundational Relaxation Deficit mineral — address it through diet first; consider low-dose supplementation only under physician guidance.
Choose Potassium if: Your cramps worsen after heavy sweating, you eat few fruits and vegetables, or a blood test confirms low potassium levels.
Skip Potassium supplements if: You have kidney disease or take ACE inhibitors — excess potassium can cause dangerous heart rhythm changes. Use food sources instead, with your doctor’s guidance.
#4 Vitamin D – Best for Deficiencies
Vitamin D surprises many people on this list — not because it directly relaxes muscles, but because it helps your intestines absorb calcium. When Vitamin D is deficient, calcium absorption drops, and the calcium-magnesium balance that governs muscle contraction and release becomes dysregulated.
Key Specs: Recommended dose for deficiency: 1,500–2,000 IU/day (D3 form preferred); always test blood levels (25-OH Vitamin D) before supplementing at high doses
Pros:
- Crucial for calcium metabolism — a deficiency can amplify cramp frequency indirectly even when calcium intake is adequate
- D3 (cholecalciferol) is the preferred supplemental form; absorbs better than D2
- Widely available, low cost, and safe at standard doses for most adults
Cons:
- A pivotal finding from PubMed research (29357208): correcting Vitamin D deficiency had no direct effect on muscle cramps — potassium and pain levels were far stronger predictors. This means Vitamin D supplementation helps only if deficiency is the underlying issue, not as a standalone cramp remedy for everyone
- Fat-soluble, meaning it accumulates in the body — excessive intake over time can cause toxicity; do not self-prescribe mega-doses
- Testing is required to know if you actually need it
Real-World Usage: Vitamin D supplementation makes the most sense in winter months, for people who work indoors, or for older adults whose skin produces less vitamin D from sun exposure. If you’ve addressed magnesium and potassium and cramps persist, a blood test for Vitamin D is a logical next step.
Verdict: Vitamin D earns its place on this list as a targeted fix for deficiency-linked spasms — but it’s not the universal muscle relaxer many supplement labels imply.
Choose Vitamin D if: Blood work confirms a deficiency, you live in a low-sunlight region, or you are over 60 and rarely outdoors.
Skip Vitamin D if: Your levels are already normal — supplementing beyond sufficiency does not reduce cramp frequency, per available clinical evidence.
#5 Vitamin B-Complex – Best for Nerves
If your spasms feel more like persistent random twitches than the deep, locking cramps of a charlie horse, a B-vitamin deficiency — particularly B12 — may be the culprit. B vitamins don’t directly relax muscles; they maintain the nerves that tell muscles when to fire. When those nerves misfire because of B12 deficiency, you get muscle twitching, cramping, and even weakness.
Key Specs: B12 (cobalamin): 1,000 mcg/day for deficiency correction; B6 (pyridoxine): 1.3–2 mg/day standard; B-complex capsule covers all eight B vitamins together
Pros:
- B12 deficiency is well-documented as a cause of neurological symptoms including muscle twitching and cramps, per NIH/PMC research on B12 deficiency
- Particularly important for vegans and vegetarians, older adults (who absorb B12 less efficiently), and anyone taking metformin (a common diabetes drug that depletes B12)
- B-complex supplements are affordable and widely available; water-soluble, so excess is excreted rather than accumulated
Cons:
- B vitamins will not help if your twitching is caused by magnesium or potassium deficiency — they target nerve health, not mineral balance
- High-dose B6 over long periods (above 100 mg/day) can actually cause nerve damage — stick to standard doses
- Blood testing for B12 levels is the only way to confirm whether this is your specific issue
Real-World Usage: Adults over 50, people on strict plant-based diets, and anyone who has been on metformin for more than a year should consider a B-complex supplement almost routinely. The link between B12 and muscle twitching is frequently missed because twitching looks less dramatic than a cramp — but the underlying nerve disruption responds well to B12 supplementation when deficiency is the cause.
Verdict: Vitamin B-complex is the right targeted fix for nerve-origin twitching and cramping in people whose magnesium levels are already adequate.
Choose B-Complex if: You are vegan, over 50, on metformin, or your spasms feel more like random twitching than deep muscle locks.
Skip B-Complex if: Your bloodwork shows normal B12 — adding more will not reduce cramps caused by mineral deficiency.
#6 Calcium – Essential Support Mineral
Calcium is the accelerator in the muscle’s two-pedal system — it triggers every contraction. Without adequate calcium, muscles can become hyperexcitable and cramp unpredictably. However, true calcium deficiency (hypocalcemia) is less common in the general population than magnesium deficiency, and supplementing calcium without attention to Vitamin D and magnesium ratios can backfire.
Key Specs: Recommended daily intake: 1,000–1,200 mg (adults); most people get 600–900 mg from diet; calcium citrate absorbs better than carbonate, especially without food
| Form | Best Taken | Notes |
|---|---|---|
| Calcium Citrate | With or without food | Better absorbed; preferred for older adults |
| Calcium Carbonate | With meals | Higher elemental calcium; requires stomach acid |
Best for: Adults who consume little dairy, are post-menopausal, or have confirmed low calcium intake alongside muscle cramping.
Not for: People with hypercalcemia (high blood calcium), kidney stone history, or those already eating a calcium-rich diet — excess calcium can worsen kidney stones and interfere with magnesium absorption.
Always consult your doctor before adding calcium supplements, particularly if you have cardiovascular concerns — some research has linked high-dose supplemental calcium to cardiovascular risk.
#7 Cramp Bark – Best Entry-Level Herb
Cramp bark (Viburnum opulus) is a traditional herbal antispasmodic (a substance that reduces involuntary muscle contractions) used for centuries in North American and European folk medicine. It contains compounds called scopoletin and viopudial that appear to relax smooth and skeletal muscle tissue, though human clinical trials remain limited.
Key Specs: Typical dose: 300–500 mg standardized extract, 2–3 times daily; available in capsule, tincture (liquid extract), and tea form
Best for: Adults who prefer a plant-based approach, experience mild to moderate spasms, and want to avoid pharmaceutical muscle relaxants.
Not for: Pregnant women (contraindicated — may stimulate uterine muscle), people with aspirin sensitivity (shares related compounds), or anyone expecting rapid relief from severe spasms.
Cramp bark earns a “Preliminary” evidence rating — its traditional use is well-documented, but large-scale RCTs in humans are lacking. Think of it as the gentlest option on this list, appropriate as a complement to mineral supplementation rather than a replacement. It bridges naturally to the fuller discussion of herbal options in the section below.
Consult your doctor or pharmacist before starting cramp bark or any herbal supplement, especially alongside prescription medications.
Magnesium Deep Dive: Glycinate, Citrate, Oxide

Magnesium is the single most important supplement for the Relaxation Deficit — and the single most confusing, because not all forms work equally well. Understanding the differences between forms prevents the most expensive and common mistake in the cramp supplement category. Magnesium oxide performs no better than placebo for nocturnal leg cramps (JAMA, 2017) — so selecting highly bioavailable glycinate or citrate is crucial for real relief.
Which Magnesium Form Works Best?
Organic magnesium salts like glycinate and citrate absorb substantially better than inorganic forms. The bioavailability of a supplement determines how much of the nutrient your intestinal cells can actually transport into the bloodstream. A 2026 PMC systematic review confirms that organic forms dissolve more readily in the gut environment. BodyMuscleMatters analysis of these organic magnesium forms shows they reliably replenish tissue levels, whereas cheap alternatives like magnesium oxide simply pull water into the intestines, causing laxative effects rather than muscle relaxation.
Here is the critical, counterintuitive finding that every other guide on this topic misses: magnesium oxide — the form found in the cheapest, most widely sold magnesium supplements — does not outperform placebo for nocturnal leg cramps.
A randomized, double-blind, placebo-controlled trial published in JAMA Internal Medicine (JAMA clinical trial, 2017) tested 94 adults with nocturnal leg cramps. Both the magnesium oxide group and the placebo group saw cramp frequency drop by roughly 3 episodes per week — but there was no statistically significant difference between them (P=0.67). In plain terms: the sugar pill worked just as well as magnesium oxide. The perceived benefit was almost entirely placebo effect.

Caption: Organic magnesium forms (glycinate, citrate) absorb far more efficiently than oxide — the JAMA RCT confirms oxide performs no better than placebo for nocturnal cramps.
| Form | Bioavailability | GI Tolerance | Best Use | Evidence for Cramps |
|---|---|---|---|---|
| Glycinate | Highest | Excellent | Daily use, sleep support | Strong |
| Citrate | High | Good (mild laxative) | Budget pick, post-exercise | Strong |
| Malate | High | Good | Fatigue + cramps | Moderate |
| Oxide | Lowest | Poor (high laxative risk) | Laxative only | Fails vs. placebo (JAMA, 2017) |
Magnesium glycinate is the best overall form for muscle spasms — highest absorption, least digestive disruption, and glycine’s calming effect as a bonus. Citrate is an excellent runner-up at lower cost. Oxide is the form to avoid specifically for cramp relief.
How Much Magnesium Should You Take?
This is the question 100% of competitor articles ignore — and the gap that leaves people guessing. Here are the evidence-based dosage guidelines:
- Standard adult dosing for muscle spasm relief:
- Start at 200 mg/day of elemental magnesium (the actual magnesium content, not the total weight of the compound)
- Target range: 300–400 mg/day for most adults — this covers the Recommended Dietary Allowance for magnesium (310–420 mg/day depending on age and sex, per NIH Office of Dietary Supplements)
- Maximum safe dose from supplements: 350 mg/day of supplemental magnesium for adults without a physician’s guidance; dietary magnesium from food has no upper limit
- Timing: Take 30–60 minutes before bed for nighttime cramps; split doses (morning + evening) for daytime muscle tension
- Duration: Allow 3–4 weeks of consistent use before evaluating effectiveness — magnesium deficiency takes time to correct
Consult your doctor before exceeding 350 mg/day of supplemental magnesium, especially if you have kidney disease or take antibiotics, heart medications, or diuretics. The FDA safety guidance advises that mixing medications and dietary supplements can have unintended and sometimes dangerous effects.
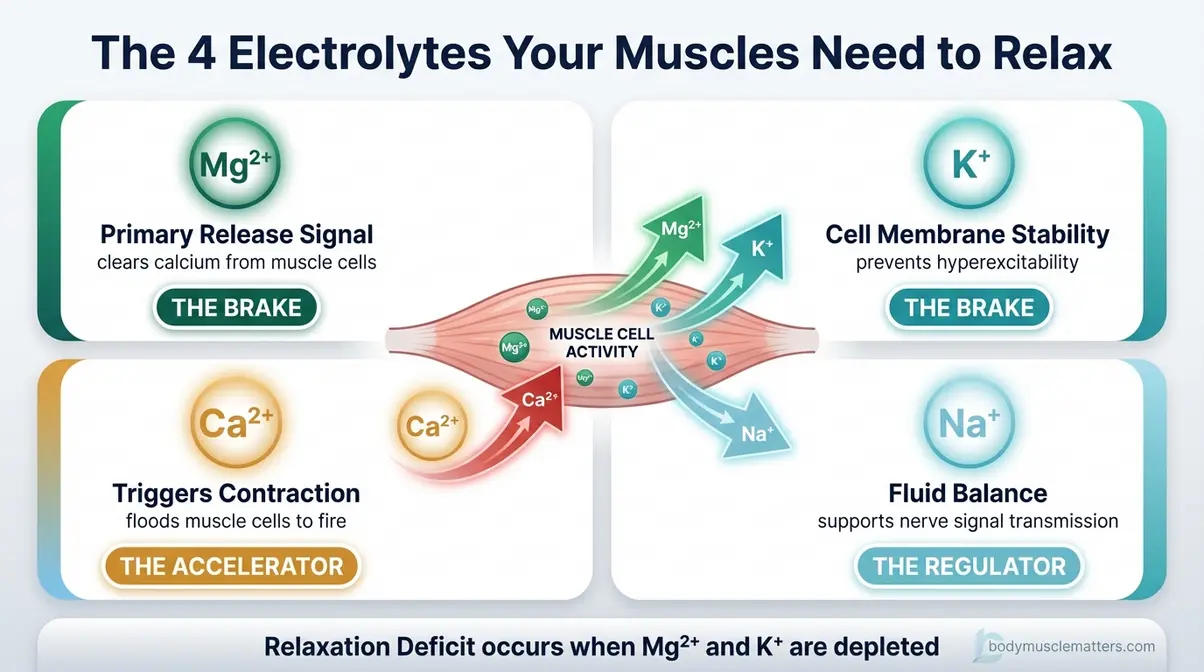
Caption: Magnesium and potassium are the primary “release” minerals — without adequate levels, muscles cannot complete the relaxation phase of a contraction cycle.
Supplements for Back Spasms & Inflammation
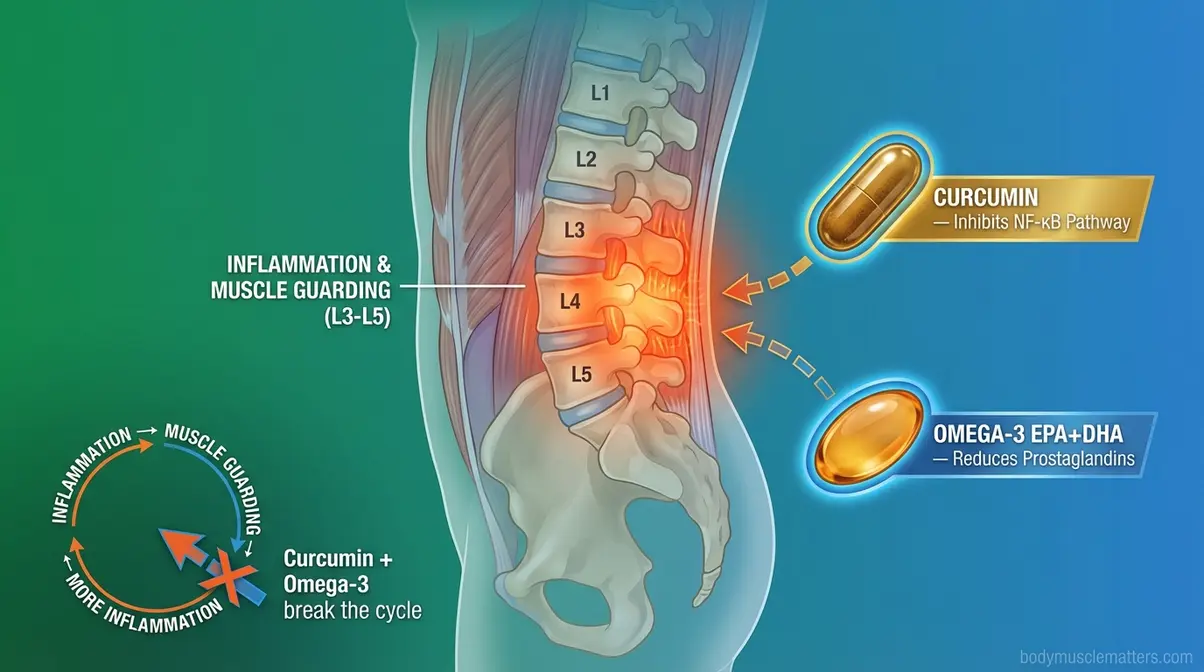
Back muscle spasms have a different character than nighttime leg cramps. They often involve a cycle of inflammation → protective muscle guarding → more inflammation — a feedback loop that mineral supplements alone may not break. Two anti-inflammatory supplements have meaningful evidence for this pattern. Black pepper extract increases curcumin absorption by up to 2,000% — so pairing these compounds is essential for effectively targeting inflammation-driven back spasms.
Curcumin & Tart Cherry for Inflammation
Curcumin delivers powerful anti-inflammatory properties that help break the cycle of back muscle spasms. Inflammation triggers protective muscle guarding, where surrounding tissues lock up around an injured area to prevent further movement. Curcumin specifically inhibits the NF-κB inflammatory signaling pathway in muscle and connective tissue. Because standard turmeric powder suffers from low bioavailability, effective back spasm protocols require curcumin supplements formulated with piperine or phospholipid complexes to ensure the active compounds reach the affected muscle tissue.
Tart cherry extract is emerging as a complementary option. Tart cherries are rich in anthocyanins (plant pigments with antioxidant and anti-inflammatory activity) that appear to reduce both exercise-induced inflammation and muscle soreness. A standard therapeutic dose is 480 mg of tart cherry extract or 8–12 oz of tart cherry juice daily. Neither curcumin nor tart cherry extract replaces magnesium for the Relaxation Deficit — they address the inflammatory layer underneath.
Consult your doctor or pharmacist before starting curcumin supplements if you take blood thinners, as curcumin can potentiate (increase the effect of) anticoagulant medications.
Omega-3 Fish Oil for Post-Exercise Pain
Omega-3 fatty acids (EPA and DHA — essential fats found in fatty fish and fish oil supplements) reduce the production of pro-inflammatory prostaglandins (hormone-like molecules that amplify pain and muscle soreness). For back spasms triggered by repeated exercise or physical labor, omega-3s address the root inflammatory signal rather than masking pain.
A standard dose of 2–3 grams of combined EPA+DHA per day is supported by the evidence for general inflammation reduction. Look for third-party tested products — fish oil supplements vary widely in actual EPA/DHA content versus label claims. Algae-based omega-3 capsules provide equivalent EPA/DHA without fish-sourced ingredients, making them appropriate for vegetarian and vegan adults.
Omega-3 + Curcumin together makes practical sense for back spasm patterns involving inflammation: curcumin tackles the NF-κB pathway, while omega-3 reduces prostaglandin signaling. This layered approach targets the inflammatory cycle from two angles simultaneously.
Caption: Back spasms driven by inflammation respond differently than mineral-deficiency cramps — curcumin and omega-3 address the inflammatory cycle that keeps muscles guarded and tense.
Natural Herbal Supplements for Muscle Relaxation

For adults who want to avoid pharmaceutical muscle relaxants — whether due to side effects, driving concerns, or personal preference — several herbal options have meaningful traditional evidence and, in some cases, preliminary clinical support. Their mechanisms differ from mineral supplements: instead of replenishing what muscles need to release, they act directly on muscle and nerve tissue to reduce excitability. Valerian extract produces a clear relaxant effect on skeletal muscle (PMC5934700, 2018) — making it the most clinically validated herbal alternative to pharmaceutical muscle relaxants.
Cramp Bark & Chamomile: Anti-Spasmodics
Cramp bark provides a traditional antispasmodic approach for adults seeking plant-based spasm relief. This herbal remedy contains active compounds called scopoletin and viopudial, which modulate calcium channels within smooth and skeletal muscle tissue. By reducing the calcium influx that triggers involuntary contractions, cramp bark directly addresses muscle hyperexcitability. While large-scale human clinical trials remain limited, generations of traditional use combined with emerging botanical research suggest it serves as a gentle, non-pharmaceutical option for managing mild to moderate muscle tension.
German chamomile (Matricaria chamomilla) shows a different mechanism. A 2018 study published in PMC (chamomile relaxant study) demonstrated that Roman chamomile extract produces a direct, prolonged smooth muscle-relaxant effect linked to its flavonoid content — specifically apigenin, a compound that modulates GABA receptors (the same calming receptor system targeted by some anti-anxiety medications). Chamomile tea before bed is a practical, low-risk entry point for anyone experiencing nighttime muscle tension.
Contraindications to note: Both cramp bark and chamomile carry a low but real allergy risk for people sensitive to plants in the Asteraceae family (ragweed, chrysanthemums, marigolds). Start with a low dose and monitor for allergic reactions. Chamomile may interact with warfarin (a blood thinner) — always disclose herbal supplement use to your pharmacist.
Consult your doctor or pharmacist before starting any herbal supplement, especially if you are pregnant, nursing, or taking prescription blood thinners.
Valerian Root for Nighttime Tension
Valerian root (Valeriana officinalis) is arguably the most clinically studied herbal relaxant for skeletal muscle. A 2018 study in PMC (valerian root research) demonstrated that a standardized valerian extract produces a clear relaxant effect on skeletal muscle in controlled conditions, reducing muscle strength metrics in a pattern similar to conventional muscle relaxants — without the sedation profile of prescription options at standard doses.
For people whose muscle spasms are worsened by stress or whose nighttime cramps prevent them from returning to sleep, valerian root addresses two problems simultaneously: direct muscle relaxation and improved sleep quality. Typical dosing is 300–600 mg of standardized extract taken 30–60 minutes before bed. Notably, studies suggest valerian’s sleep effects build over 2–4 weeks of consistent use — it is not an “as-needed” acute relief option.
Bioavailability risks: Valerian interacts with CNS depressants (alcohol, benzodiazepines, sleep medications) and can cause excessive sedation when combined. It is not appropriate for daytime use if you need to drive or operate machinery.
Caption: Valerian root has the strongest published evidence for skeletal muscle relaxation among herbal options — PMC5934700 confirms a direct relaxant effect comparable to mild pharmaceutical muscle relaxants.
OTC Medicines & Baclofen for Muscle Spasms
Supplements address the Relaxation Deficit over time — but some spasms are severe, acute, or disease-related enough to require faster-acting pharmaceutical options. Understanding where over-the-counter (OTC) medications and prescription drugs fit in the picture is part of making a genuinely informed decision. Oral baclofen achieves complete cramp resolution in 72% of patients (PubMed, 2016) — providing a powerful prescription fallback when over-the-counter supplements prove insufficient.
OTC Options for Acute Muscle Spasms
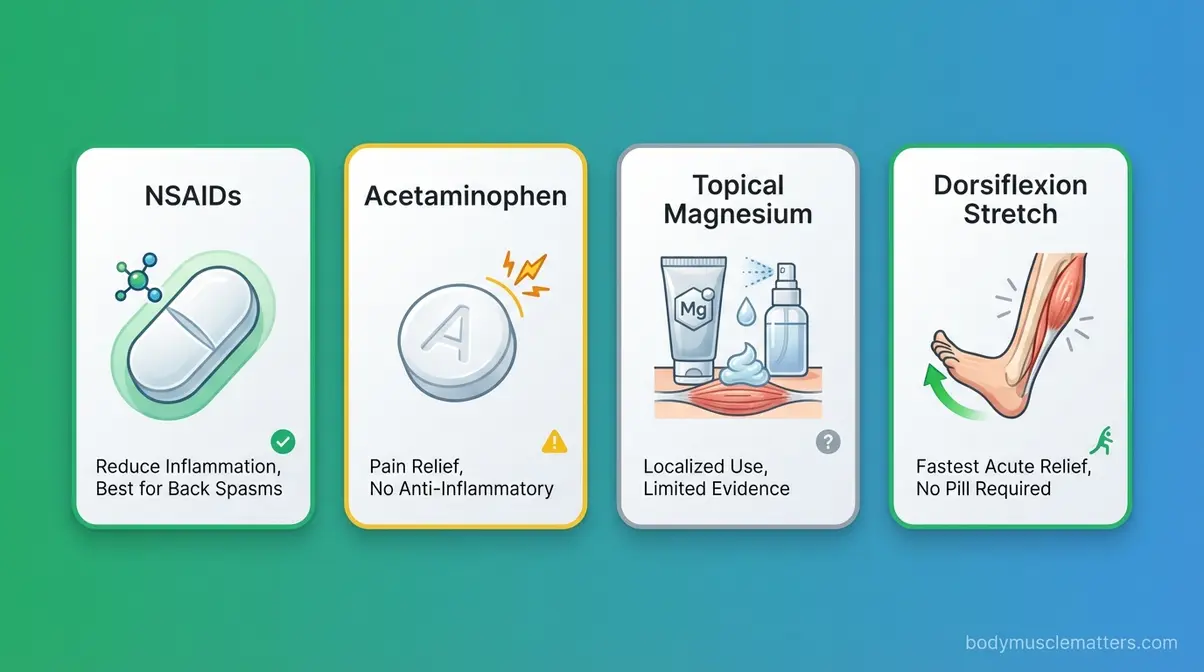
No OTC drug is specifically FDA-approved as a muscle relaxant for general spasm use. However, several commonly available medications help manage pain and inflammation that worsen spasm cycles:
- NSAIDs (ibuprofen, naproxen): Reduce inflammation and associated muscle guarding. Most useful for back spasms and post-exercise cramps. Follow package dosing instructions — chronic use carries GI and cardiovascular risks.
- Acetaminophen (Tylenol): Manages spasm-related pain without anti-inflammatory effects. A reasonable choice when NSAIDs are contraindicated.
- Topical magnesium sprays and gels: Some users report relief from transdermal (through-the-skin) magnesium products for localized cramps. Evidence is limited — absorption through skin is substantially lower than oral supplementation — but they carry minimal risk.
For acute nighttime charlie horses, the fastest non-pharmacological relief is forceful dorsiflexion (pulling your toes toward your shin while straightening your knee). This stretches the calf and mechanically interrupts the contraction-without-release cycle of the Relaxation Deficit in real time.
Baclofen: For Severe or Chronic Spasms
Baclofen operates as a prescription-only GABA-B receptor agonist that suppresses overactive nerve signals. This pharmaceutical muscle relaxant mimics the brain’s primary calming neurotransmitter, specifically targeting the spinal cord pathways that drive involuntary muscle contractions. FDA-approved for chronic spasticity conditions like multiple sclerosis, baclofen delivers dramatic clinical outcomes that over-the-counter supplements cannot match. Medical supervision remains essential, as the medication carries significant side effects and requires careful dosage tapering to avoid withdrawal complications. It represents the ultimate step up for severe spasm management.
The clinical outcomes are meaningful. A randomized placebo-controlled trial published in PubMed (PubMed baclofen trial) found that oral baclofen at 30 mg/day achieved complete cramp resolution in 72% of patients — a dramatic result compared to any OTC option. Reduction in frequency, severity, and duration of cramps were all statistically significant (P<0.001 for severity and duration). Baclofen was well-tolerated, though cramps returned after discontinuation.
Baclofen is not a supplement and is not available without a prescription. Common side effects include drowsiness, dizziness, and weakness — particularly at the start of treatment. Abrupt discontinuation can trigger withdrawal seizures; always taper under physician supervision. Baclofen is appropriate only for people with severe, chronic spasms that have not responded to conservative approaches, and should be prescribed and monitored by a physician.
This is not a decision you should make alone. If your spasms are severe enough that you are considering a prescription muscle relaxant, that is a conversation for your doctor — not a supplement guide.
The FDA warns explicitly that mixing medications and dietary supplements can have dangerous, unintended effects. Always disclose all supplements to your prescribing physician.
How to Choose the Right Supplement
Understanding the Relaxation Deficit makes every supplement on this list logical — but the best choice depends on your specific spasm pattern. Use the decision matrix below to find your starting point, then build from there. Creating a layered supplement protocol yields the highest success rate for chronic spasms. The most effective approach begins with a strong foundation of magnesium glycinate and dietary potassium to address the baseline Relaxation Deficit. BodyMuscleMatters guidelines suggest observing outcomes for four weeks before adding targeted support like B-complex vitamins for nerve twitches or curcumin for inflammatory back pain. This systematic methodology ensures you only take the supplements your body actually needs, minimizing costs and reducing the risk of nutrient imbalances.
Decision Matrix by Symptom Type
| Your Situation | First Choice | Add-On | What to Avoid |
|---|---|---|---|
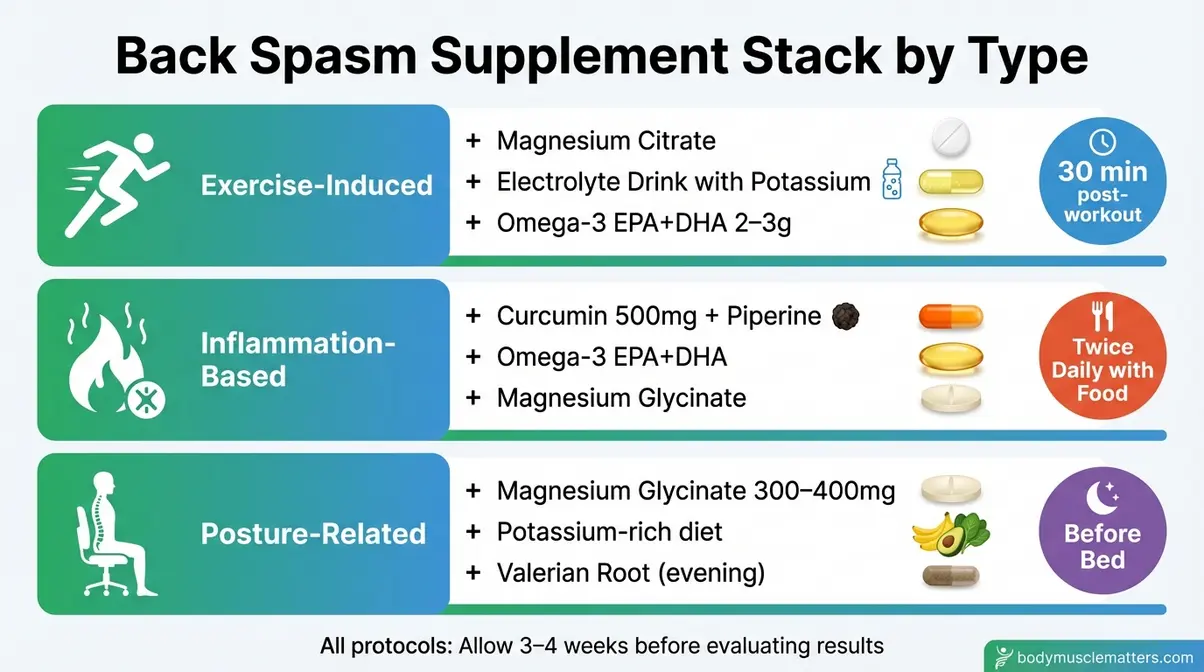
| Nighttime charlie horses, waking from sleep | Magnesium Glycinate 300–400 mg before bed | Potassium-rich diet | Magnesium Oxide (fails vs. placebo) |
| Exercise-induced cramps during/after workouts | Magnesium Citrate + Electrolyte Drink | Potassium + Sodium | High-dose calcium without magnesium balance |
| Random muscle twitching throughout the day | Vitamin B-Complex (test B12 levels first) | Magnesium Glycinate | Assuming magnesium alone resolves nerve-origin twitching |
| Back spasms with inflammation and stiffness | Curcumin + Omega-3 Fish Oil | Magnesium Citrate | Relying solely on NSAIDs long-term |
| Deficiency-linked spasms (confirmed by bloodwork) | Vitamin D (if deficient) + Potassium | Magnesium Glycinate | Mega-dosing Vitamin D without testing |
| Herbal preference, mild evening tension | Valerian Root + Chamomile Tea | Magnesium Glycinate | Combining valerian with alcohol or sleep medications |
| Severe, chronic, or disease-related spasticity | Consult physician (Baclofen if prescribed) | Medical guidance | Self-treating with OTC supplements alone |
Caption: Your spasm type determines your best supplement — nighttime charlie horses point to the Relaxation Deficit (magnesium + potassium), while daytime twitching often signals nerve-origin B-vitamin deficiency.
Your Personal Supplement Protocol
Most adults experiencing recurring spasms benefit from a layered approach rather than a single supplement. Here is a practical starting framework built around the Relaxation Deficit principle:
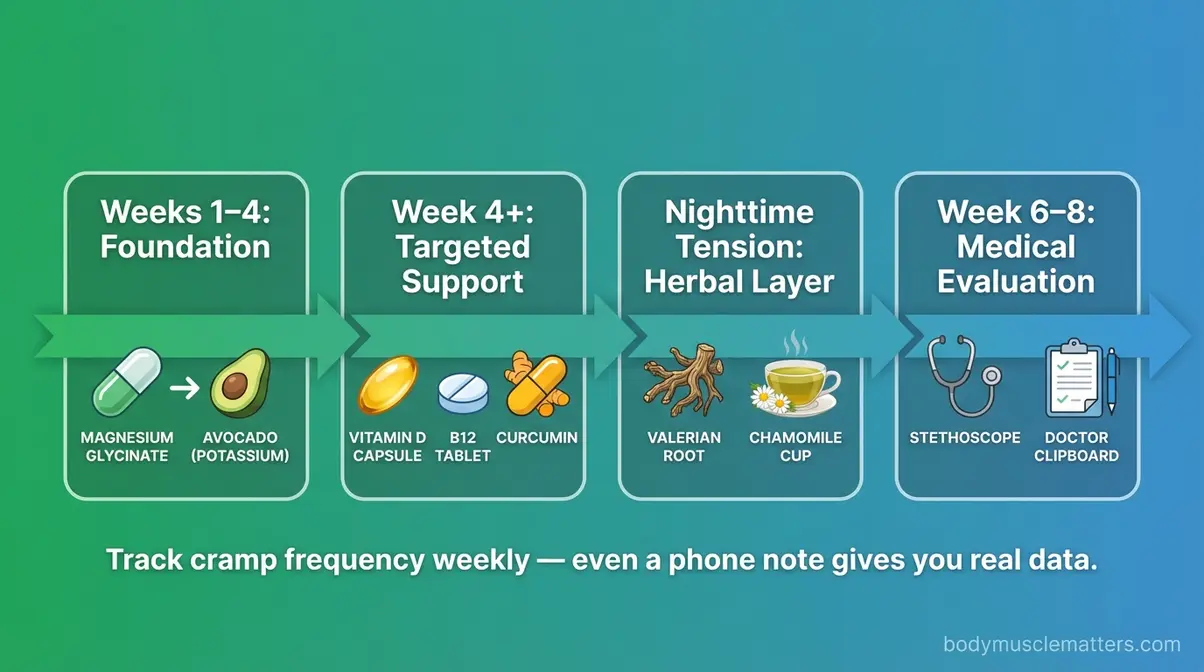
Step 1 — Start with the foundation (Weeks 1–4):
Begin with magnesium glycinate (200 mg/day, increasing to 300–400 mg after one week if tolerated). Add potassium through food — one avocado or medium sweet potato daily easily adds 700–900 mg of potassium without pills. Assess cramp frequency after four weeks.
Step 2 — Add targeted support (Week 4 onward):
If nighttime cramps persist, confirm your Vitamin D and B12 levels via a blood panel. Add deficient nutrients specifically. If back spasms are prominent, layer in curcumin (500 mg twice daily with piperine) and omega-3 fish oil (2 g EPA+DHA daily).
Step 3 — Consider herbal options for nighttime tension:
If sleep disruption from muscle tension is a major issue, valerian root (300–600 mg before bed) complements magnesium glycinate without significant interaction risk at standard doses. Chamomile tea is a low-risk addition at any time.
Step 4 — Seek medical evaluation if needed:
If spasms remain severe after 6–8 weeks of consistent supplementation — or if they are accompanied by weakness, numbness, significant pain, or visible muscle wasting — consult a physician. Some underlying conditions (thyroid disorders, peripheral artery disease, medication side effects) cause cramps that supplements cannot address.
Consult your doctor or pharmacist before starting any new supplement, especially if you take prescription medications.
Risks, Side Effects, and When to See a Doctor
Honest guidance about risks is the mark of genuinely useful health information. Every supplement on this list carries a side effect profile — and some carry real drug interaction risks that matter significantly for certain people. Supplemental potassium can trigger dangerous heart arrhythmias in patients with kidney impairment — meaning dietary sources remain the safest option for most adults.
Side Effects & Drug Interactions
Drug-supplement interactions represent a serious risk factor when treating muscle spasms. Common muscle-relaxing minerals like magnesium can significantly reduce the absorption of certain antibiotics and osteoporosis medications if taken simultaneously. Furthermore, herbal remedies like valerian root and chamomile amplify the sedative effects of alcohol, anti-anxiety drugs, and prescription sleep aids. Consulting a qualified pharmacist or physician before starting any new supplement protocol ensures these products will not dangerously interfere with your existing prescription medications or underlying health conditions.
Magnesium — The most common side effect at higher doses is diarrhea (particularly with oxide and citrate). Magnesium can reduce the absorption of some antibiotics (tetracyclines, fluoroquinolones) and bisphosphonates (osteoporosis drugs) — take magnesium at least 2 hours apart from these medications. People with kidney disease should not supplement magnesium without physician approval, as damaged kidneys cannot clear excess magnesium effectively.
Potassium — Supplemental potassium at doses above dietary levels can cause dangerous heart arrhythmias (irregular heartbeat) in people with kidney impairment or those taking potassium-sparing diuretics (like spironolactone) or ACE inhibitors. This is a serious interaction, not a theoretical one — per medical guidance, high potassium can affect heart rhythm even in otherwise healthy adults if accumulated too quickly.
Vitamin D — Fat-soluble and accumulates in the body. Toxicity from excessive supplementation can cause hypercalcemia (dangerously high blood calcium), resulting in nausea, kidney damage, and cardiac issues. Never self-prescribe doses above 4,000 IU/day without physician guidance.
Valerian Root and Chamomile — Both interact with CNS depressants including alcohol, benzodiazepines, and sleep medications. The FDA explicitly cautions that herbal supplements can interact with prescription medications in ways that are difficult to predict. Chamomile may potentiate warfarin.
Curcumin — Potentiates blood thinners (warfarin, aspirin, clopidogrel). Not recommended in high doses during pregnancy.
Warning Signs for Medical Attention
Muscle spasms are usually benign and manageable. However, certain patterns are warning signs that require prompt medical evaluation — not more supplements:
- Spasms accompanied by muscle weakness or atrophy (visible shrinking) — may indicate a neurological condition or motor neuron disease
- Cramps in unusual locations (hands, face, throat) rather than the typical legs and feet — can signal electrolyte emergencies or thyroid disease
- Spasms that are painful enough to wake you every night and don’t improve after 4–6 weeks of magnesium supplementation — warrant a blood panel including calcium, potassium, magnesium, B12, and Vitamin D
- New or worsening spasms after starting a new medication — statins, diuretics, and some blood pressure drugs commonly deplete magnesium and potassium as a side effect
- Visible muscle contractions visible under the skin (fasciculations) that spread or worsen — should be evaluated by a neurologist
- Any spasm associated with chest pain, shortness of breath, or facial droop — call emergency services immediately
Frequently Asked Questions
What’s the best supplement for spasms?
Magnesium glycinate is the best overall supplement for most adults with muscle spasms, according to evidence from NIH and peer-reviewed research on magnesium bioavailability. It addresses the Relaxation Deficit directly by replenishing the mineral your muscles need to release after contracting. A dose of 200–400 mg of elemental magnesium glycinate daily, taken in the evening, covers the most common cause of recurring cramps and is well-tolerated for long-term use. Potassium, whether through food or supervised low-dose supplementation, is the most important add-on for people who also sweat heavily or eat few fruits and vegetables. Be sure to avoid magnesium oxide specifically, as a JAMA RCT (JAMA Internal Medicine, 2017) showed it performed no better than placebo for nocturnal leg cramps.
What vitamin lack causes muscle spasms?
Multiple nutrient deficiencies can cause muscle spasms, with magnesium deficiency affecting nearly 50% of U.S. adults by dietary intake standards (NHANES data, IMR Press, 2026). While Vitamin D deficiency disrupts calcium metabolism, research from the Physical Therapy Journal in 2018 found that dietary potassium was actually a stronger predictor of cramp presence than Vitamin D. Additionally, Vitamin B12 deficiency causes nerve-origin twitching rather than classic cramps, making it the primary suspect for people experiencing persistent daytime muscle twitching.
What nutrients stop muscle spasms?
The four nutrients most directly linked to stopping muscle spasms are magnesium, potassium, calcium, and Vitamin B12. Magnesium and potassium act as the primary “release” minerals in the Relaxation Deficit framework, signaling muscles to relax after contraction. Calcium serves as the contraction mineral, meaning adequate levels are essential, but excess calcium without sufficient magnesium can actually worsen spasms. Finally, Vitamin B12 supports the nerve pathways that control muscle signaling, and addressing all four through diet and targeted supplementation covers the most common deficiency-driven spasm patterns.
What vitamin acts like a muscle relaxer?
Magnesium is often called “nature’s muscle relaxant” because it directly regulates the calcium channels that control muscle contraction and release. Functioning as the physiological brake in the muscle’s contraction cycle, magnesium allows muscles to stop firing. Among true vitamins, Vitamin B6 supports the synthesis of GABA, which is the brain’s calming neurotransmitter that may reduce nerve-driven muscle hyperexcitability. Herbal options like valerian root also work similarly to a mild relaxer by modulating GABA receptors, producing a direct skeletal muscle relaxant effect. While none of these match the potency of prescription muscle relaxants, they safely address the underlying deficit without severe side effects.
Does B12 stop muscle spasms?
Vitamin B12 can successfully stop muscle twitching and spasms when a B12 deficiency is the underlying cause, but it won’t help if your symptoms stem from low magnesium or potassium. Because B12 maintains the protective myelin sheath around nerve fibers, a deficiency causes nerve signals to misfire, producing rapid, random muscle twitches that differ from deep charlie horses. A blood test for serum B12 is the only reliable way to confirm whether this supplementation is appropriate for your specific nerve-health situation.
Limitations and When to Consider Other Approaches
Common Pitfalls
Pitfall 1: Buying magnesium oxide because it’s cheap. The JAMA RCT data is unambiguous — oxide performs no better than placebo for nocturnal leg cramps. Paying less for a form that doesn’t work is not a bargain; it’s a waste.
Pitfall 2: Expecting results overnight. Magnesium deficiency takes weeks to develop and weeks to correct. Adults who try glycinate for three days and conclude “it doesn’t work” have not given the supplement enough time to shift their baseline mineral levels. Commit to 3–4 weeks of consistent use before evaluating.
Pitfall 3: Mega-dosing a single mineral without balance. High-dose calcium without adequate magnesium can actually worsen spasms by throwing the contraction-relaxation ratio further out of balance. High-dose potassium supplementation without physician oversight carries cardiac risk. The mineral system is a balance — not a dial to be turned up on one nutrient alone.
Pitfall 4: Using herbal relaxants with CNS depressants. Combining valerian root or chamomile with alcohol, sleep medications, or anti-anxiety drugs amplifies sedation in ways that can become dangerous — particularly for older adults.
Pitfall 5: Ignoring medication side effects. Statins (cholesterol-lowering drugs) are among the most common causes of drug-induced muscle cramps and weakness. If your cramps began after starting a new prescription, talk to your prescribing physician before adding supplements.
When to Choose Alternatives
When spasms are disease-driven: Conditions like multiple sclerosis, ALS, peripheral artery disease, or hypothyroidism cause cramps that respond only to treatment of the underlying disease — no supplement addresses these at the root.
When cramps are medication-induced: Diuretics deplete both magnesium and potassium. Statins disrupt the CoQ10 pathway in muscle cells. In these cases, managing the medication side effect (with your doctor) is more appropriate than adding more supplements.
When symptoms are severe or worsening: If cramps are debilitating, accompanied by weakness, or worsening over time, prescription options like baclofen offer meaningfully stronger clinical outcomes (72% complete resolution in the published RCT) than any OTC supplement.
When to Seek Expert Help
- Consult a physician rather than self-treating with supplements when:
- You experience spasms more than 3–4 nights per week that do not improve after 6 weeks of magnesium supplementation
- Spasms involve weakness, visible muscle wasting, or spreading fasciculations (random visible muscle ripples)
- You have chronic kidney disease, heart rhythm disorders, or take multiple prescription medications
- You are pregnant (several supplements and herbs on this list have specific pregnancy contraindications)
- Spasms are in unusual locations (face, hands, throat) rather than the typical legs and feet
The Relaxation Deficit framework makes one thing clear: most recurring muscle spasms are a solvable mineral and nerve-nourishment problem, not a permanent condition you have to endure. Magnesium glycinate addresses the core deficit for the majority of adults. Potassium, B vitamins, and targeted anti-inflammatory supplements fill in the gaps based on your specific pattern.
Start with the magnesium glycinate and potassium-from-food foundation. Give it four weeks. Track your cramp frequency — even a simple note on your phone (“2 cramps this week vs. 7 last week”) gives you real data to work from. If results are incomplete, revisit the Decision Matrix to identify whether inflammation, nerve health, or an underlying deficiency is the remaining driver.
The best next step is a conversation with your doctor or pharmacist — share the supplements you’re considering, bring your medication list, and ask for a basic blood panel covering magnesium, potassium, Vitamin D, and B12. That single panel costs less than two months of supplements and tells you exactly where your Relaxation Deficit is deepest.


